Consumer Directed Health Plans have received much criticism for the ways in which they can limit employees’ access to healthcare. But the use of incentives to reward healthy behavior can overcome these limitations.
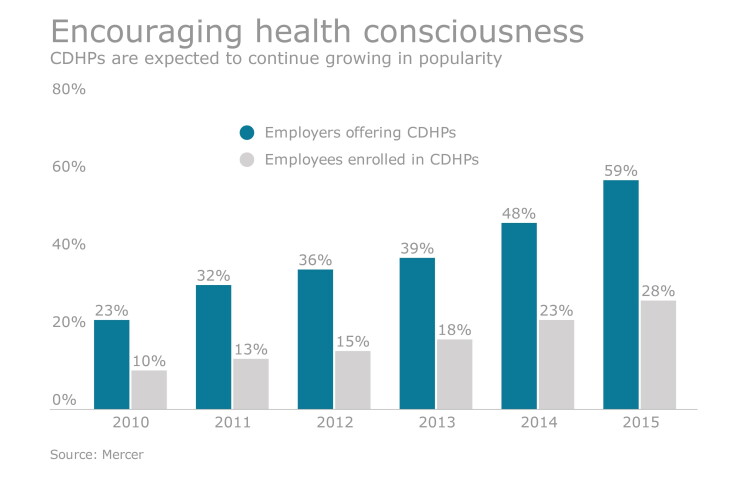
Given the continued rise in healthcare costs, CDHPs are becoming increasingly common as a cost containment strategy. Yet there are concerns that the high deductibles associated with these plans restrict access to necessary healthcare services by forcing employees to bear a greater share of the costs.
The truth is that CDHPs are just a tool. It’s how the tool is used that will determine the outcome and the level of success. Simply implementing these programs to alleviate employer costs is short sighted and misses the opportunity to introduce healthy behaviors into the mix.
It’s true that in order to encourage smart consumer-like thinking, employees need some skin in the game, and that without having to shoulder a significant share of the costs employees have little motivation to change their healthcare consumption behavior. That’s where the use of incentives, based on the validated completion of healthy behaviors, can drive positive outcomes for both employers and employees.
Many CDHPs include Health Savings Account (HSA) or Health Reimbursement Arrangement (HRA) contributions in an attempt to soften the blow of shifting costs to employees. Although it may seem counter-intuitive, making employees earn these contributions through validated actions can produce a win-win for both parties:
By providing significant financial incentives for achieving health goals, employers encourage positive behaviors and demonstrate that they care about their employees’ health and wellbeing.
From an employee perspective, out-of-pocket expenses can be significantly reduced—if the employee is willing to adopt healthy habits. This provides the employee with additional funds to pay claims, even as it helps the individual reduce the likelihood that he or she will need to file a claim in the first place. There is no better way to decrease out of pocket expenses like deductibles and copays than by avoiding them altogether.
"The one-two punch of a cost shift plus behavior changes may appear on the surface to be rough on employees."
The one-two punch of a cost shift plus behavior changes may appear on the surface to be rough on employees. However, some tough love is needed to get at the root of the problem (unhealthy behaviors), rather than simply addressing the symptom (rising health costs).
From a consultant’s perspective, recommending a CDHP without also rewarding healthy behaviors, can be short sighted and turn into a “one-time” cost-shifting exercise. By motivating employees to alter their behavior, employers can begin to improve their organizational culture and long-term risk profile. Plus there’s an added bonus: Advisers and their clients will also be collecting data that can either be analyzed against actual claims costs or can be used as part of their renewal negotiations with carriers.
So the next time you suggest a CDHP strategy, help that employer improve the health of its workforce by pairing it with a strategy to increase healthy behaviors.








