Health plan representatives are always saying that their plans are doing everything they can to control costs and deliver greater value. But then nothing ever seems to change.
The truth is that group health plans typically earn a percentage of total claims, and it is in their interest for healthcare to cost as much as possible. Employer or union group health plans are frequently associated with a variety of services — e.g., health IT, pharmacy benefit management, case management, reinsurance — each with its own revenue stream. By choosing and incentivizing vendors, plan administrators directly influence their systems’ capabilities to manage risk. Intentionally meek approaches to healthcare risk management result in excessive care and cost, in turn fueling higher expenditures, greater net revenues and elevated stock prices.
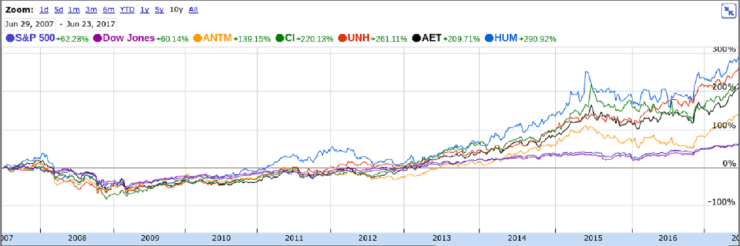
This structure has been spectacularly successful for the health insurance industry. Using data pulled from Google Finance, the chart and table below show the 10-year stock price performance of five commercial health plans: Aetna, Anthem, Cigna, Humana and United, as well as the Dow and Standard & Poor’s Index.
Stock prices began to creep upward in November 2008, when a Democratic majority was elected to Congress, foreshadowing the successful passage of the Affordable Care Act. Lobbying by healthcare interests was intense during this period, with Congress accepting an unprecedented $1.2 billion in campaign contributions, presumably in exchange for influence over the shape of the law. In the 8 years between May 2009 and May 2017, the stock prices of these insurers soared between 387 and 748 percent. They vastly outperformed the rest of the market, growing 1.5 to 3.0 times faster than the S&P and 1.2 to 2.4 times faster than the Dow.

Grim implications
Growth, driven by an endless rise in expenditures, has profoundly grim implications. Let’s say a clinical risk management firm emerges that, within a high value niche, consistently delivers measurably better health outcomes at half the cost. Reductions in unnecessary surgeries, imaging and drugs would likely yield strong savings. But the resulting drop in health plans’ net revenue would also translate into lower stock prices and market capitalization, and lead to strained relations with network providers, whose utilization and revenues would also suffer. Under these circumstances, concerns about compromised network performance and reduced valuation would deter insurers from investing in the risk management firm’s capacity to deliver better value.
Of course, these dynamics are not unique to health plans. Virtually every healthcare organization —including physician practices, health systems, imaging centers, labs, drug manufacturers, pharmacy benefit management firms — earns a percentage of the spend within its niche. Not surprisingly, each also has developed mechanisms to promote the highest possible unit volumes and pricing.
This may seem like an obvious point, but it is critical to U.S. health policy going forward. For decades, lawmakers have done the bidding of health industry lobbyists and avoided payment methodologies that reward value. This has made American healthcare, at double the cost of other developed countries, unaffordable and inaccessible to large swaths of the American people. The need to continually pay more for healthcare has drained funding away from other critical needs, such as education, transportation and infrastructure. This has played a significant role in crushing the American dream for the middle class and compromising U.S. global competitiveness and economic security.
Alternative approaches like a single payer health plan won’t solve this problem unless how healthcare is purchased also changes. A stable, sustainable health system will remain a pipedream until people refuse to pay for products and services at ever decreasing value. Instead, healthcare purchasers must tie payment to observably better results. An abundance of market-based evidence shows this is readily achievable.
Brian Klepper PhD is a healthcare analyst and a Principal of Worksite Health Advisors.









