With the fate of healthcare reform in limbo, new research suggests employers are moving forward with a host of incremental changes to their health and wellness plans in hopes of curtailing costs on their own.
Kim Buckey, VP of client services at DirectPath, an employee engagement and healthcare compliance technology company, has noticed a slowdown in adoption of high-deductible health plans and cost-shifting strategies that aren’t quite living up to expectations. DirectPath’s 2017 Medical Plan Trends and Observations Report, based on an analysis of about 975 employee benefit health plans, found employers applying creative methods for cost control.
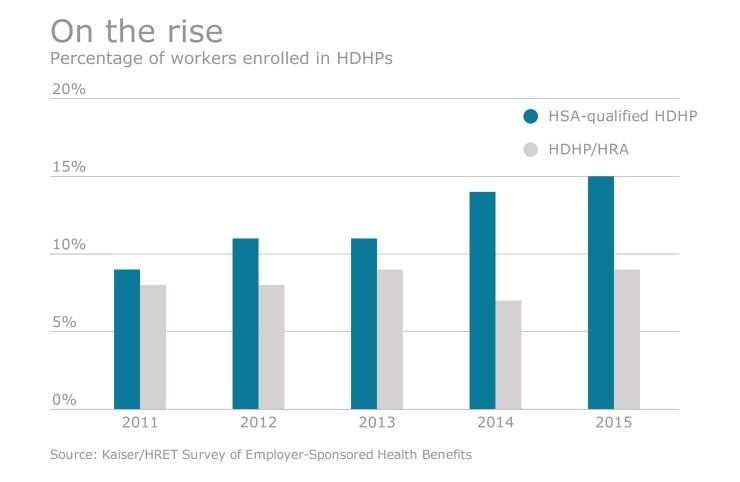
Buckey noted greater use of health savings accounts, wellness incentives, price transparency tools and alternative care options.
Slightly more than half of the employers studied by DirectPath offer a
In an effort to reduce costs and the administrative burden of tracking coverage for dependents, surcharges on spouses who can elect coverage elsewhere soared more than 40% within the past year to $152 per month.
The number of plans that offer wellness incentives rose to 58% from 50% between 2016 and 2017. Rewards included paycheck contributions, plan premium discounts, contributions to HSAs and health reimbursement arrangements and reduced co-pays for office visits.
Barriers to care and cost containment
A separate survey conducted by CEB, a technology company that monitors corporate performance, noted that although as many as one-third of organizations offer telemedicine, more than 55% of employees aren’t even aware of their availability and nearly 60% believe they’re difficult to access.
Also see: “
DirectPath and CEB both found that the average cost of specialty drugs increased by more than 30%. This reflects research conducted by the National Business Group on Health. Nearly one-third of NBGH members said the category was their highest driver of healthcare costs last year.
The pursuit of a panacea for rising group health costs has been meandering. When Buckey’s career began, she recalls how indemnity plans gave way to HMOs and managed care, then HDHPs, consumer-directed plans and private exchanges. “There is no one silver bullet that’s going to solve this problem,” she explains, “and I think employers and their advisers are starting to understand that it’s got to be a combination of things.”
More employers are now realizing that cost-shifting isn’t a viable long-term solution and that “whatever changes are put in place will require a well thought-out, year-round and robust communication plan,” she says.
There’s also a serious need to improve healthcare literacy, with Buckey noting that many employees still struggle to understand basic concepts such as co-pays, deductibles and HSAs. Consequently, she says it’s no wonder why they often “just shut down and do whatever their doctor tells them.









