Wellness programs … long the silver bullet to crushing healthcare costs and making offering benefits to employees more affordable. This has been in the benefit world vernacular for well over a decade, so why are we not seeing the impacts of this? Sure, there are some employers that do it really well, and there are wellness program vendors that tout huge ROIs, but I argue if all this were true, wellness would be the rule, not the exception.
So what are the problems with wellness programs, at least as they exist today? First, wellness programs are most attractive to those that are already well. If the employer gives incentives for someone to take 10,000 steps a day, and they are already averaging 8,000, it is not a huge leap, or huge improvement in health, to get there. But when I was 120 lbs overweight, 10,000 steps per day was such an unrealistic goal that I would not even try. Of course, you could tier the incentives and push for improvement, but now you are talking about an exponential increase in administrative overhead. And while the benefits of being more active are undisputed, a walking program is unlikely by itself to have tremendous results.
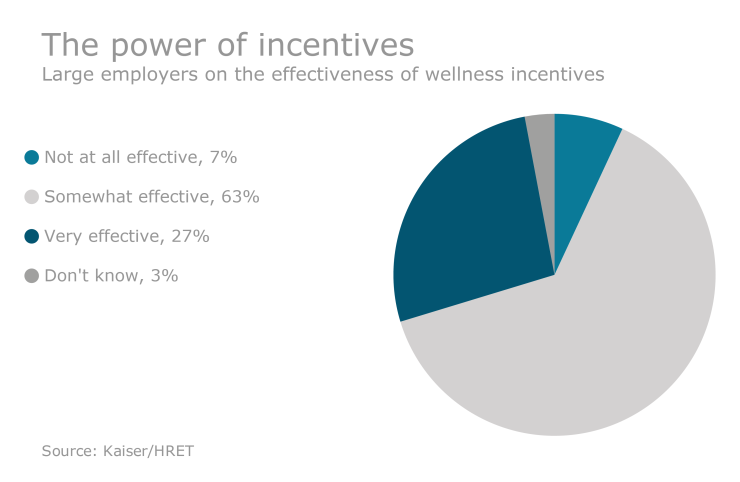
There are, of course, other wellness programs out there. Ones that identify those suffering from chronic conditions and offer to help better manage those, for example. And when employees engage in those programs, they are effective. But the engagement level is so low, that it too fails to have the overall impact we need to make health insurance more affordable.
A RAND study done in 2013 found that 32% of employers had below a 20% completion of just a health risk assessment. If employees are unwilling to even do what’s needed to identify their health issues, what chance do employers have of having an impact on them? According to that study, in large employer wellness plans that are exceptionally well managed, 55% participation is the high side of average. When you look at the percentage of employees with identified health risks that participate in the program, the numbers plummet to the low single digits for most risk factors. This reinforces what I said earlier about the “well” employees being most apt to participate.
The most telling stat from that study is this: Even in the best year, the wellness program is attributed with saving only $11.12 per member in the program per month. One study by BCBS of Kansas City found that employers in that state that participated in wellness programs saw an increase of $600 per year in costs.
The strongest evidence that wellness isn’t working is that neither employers nor employees say their plans are affordable, regardless of the wellness program’s success. None of them report a regular, sustained flat line rate trajectory, or even, heaven forbid, a decrease.
And perhaps the most challenging of all is that the majority of employers are fully insured. In a fully insured environment, there is a questionable link to reduced claims and insurance savings, and the reporting available to prove the wellness theory is woefully lacking. Plus, the Affordable Care Act creates a perverse incentive for insurance companies to want healthcare costs to go up, not down. For non-insurance geeks, allow me to explain. Insurance companies must spend 85 cents of every dollar on medical costs as a result of the “Medical Loss Ratio” provision of the ACA. Prior to this, the carrier’s profit was premium minus claims. So they were incentivized to control costs. Now, if they do that well, they have to provide a refund to the individuals and/or employers on the plan.
And lastly, wellness programs neglect one glaring fact. We all consume care at some point, and the care we consume in the U.S. continues to decline in quality and increase in cost (one example is the World Health Organization, which currently ranks our healthcare system 37th in the world, on par with Slovenia.)
There will be better solutions. We are already seeing tools that start to bring a level of transparency on both price and quality to the forefront. When looking up metrics like these are as easy as researching restaurants in a foreign city on your mobile phone, real change can start to occur. Everyone directs their anger at insurance companies, and I understand why. They raise premiums, lower benefits, and narrow networks. But worsening insurance is not the cause of the problem, but rather the result. And the answer lies in addressing the underlying factor for 85% of our premiums – the actual cost and quality of care. The biggest challenge in this is a shift in thinking – getting the employee, in this case the patient, to apply value-based metrics to their healthcare buying decisions. If we can make our healthcare high quality and low cost, then we can make the financial vehicle that pays for it the same. Until then, it cannot happen.









