The
While the proposed deal reflects the trend among insurers “to bring prescription benefit management in-house to better integrate pharmacy and medical management and to gain greater leverage in drug price negotiations,” says Brian Marcotte, National Business Group on Health president and CEO, employers are generally not optimistic that will be the case.
Only a quarter of employers say they’re optimistic that mergers between health plans and PBMs will have a positive impact on cost, quality and consumer experience, according to
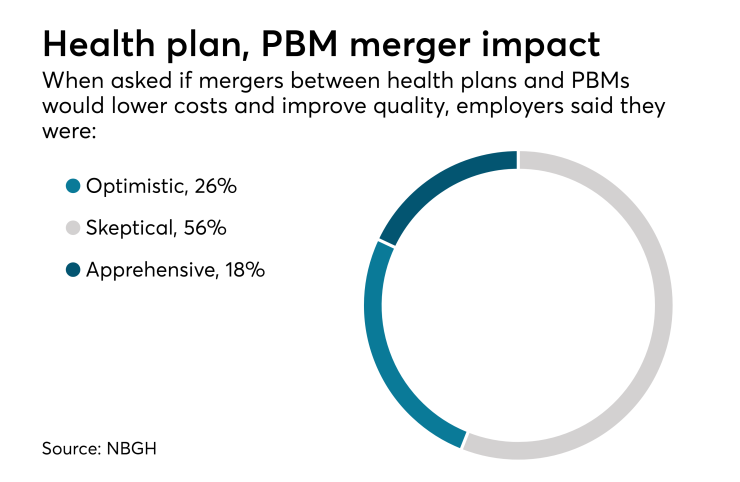
“While the deal is being held up as a way for the firms to improve care for patients and lower healthcare costs, it could do the opposite,” says Kim Buckey, vice president of client services at DirectPath, an employee engagement and healthcare compliance technology company. “The deal creates less competition, drives prescription costs and could mean decreased price transparency.”
For example, if consumers have medical insurance through Aetna, but prescription drug coverage through Express Scripts, Express Scripts may not be inclined to share drug price information with Aetna customers, she cautions.
Marcotte says there might be a more positive employer impact, but that will depend on “Cigna’s ability to execute.”
“To the extent that it results in better integration and coordination of medical and pharmacy management, it should drive better care for patients and lower costs for employer plans,” he says.
There is an opportunity to leverage scale and data from the combined entities to transform pharmaceutical supply chain contracting and adopt more sustainable, affordable and transparent prescription drug pricing models, allowing drugs to compete solely on comparative effectiveness and price, he adds.
DOJ’s antitrust division found that after the Cigna-Express Scripts merger, there will still be at least two large pharmacy benefit management firms and several smaller PBMs in the market. The DOJ added it would be hard for Cigna to increase PBM costs for other insurers because of competition from other integrated insurer-PBM players. UnitedHealth Group is currently the largest integrated health and pharmacy benefits firm, but Anthem is building its own PBM unit.
Cigna’s deal for Express Scripts came on the heels of CVS Health’s
The recent spate of mergers represents a rapidly changing market, says Marcotte, adding that it’s “too soon” to tell the overall impact it will have on employers and consumers.
“Follow through will be important to ensure that the potential benefits of this and similar mergers ultimately reach patients and employers who pay for care,” he says. “Employers that are planning to place their plan administration out to bid in the next few years will want to consider and evaluate all new combinations as the market evolves.”









