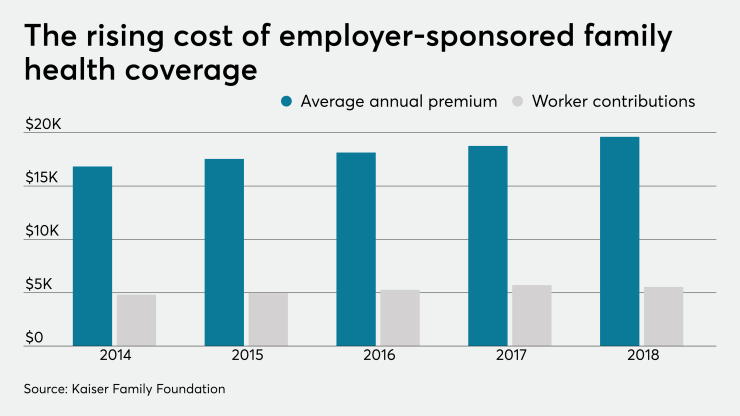The total cost of healthcare for employees and dependents, including premiums and out-of-pocket costs, is estimated to average $14,800 per employee in 2019 — up more than $700 from last year, according to recent
In the past, employers have attempted to stem the tide of these rising costs by introducing new plans and programs and shifting more of the cost of coverage and care onto employees. However, additional research shows an increasing recognition that these changes may have the opposite of the desired effect. Employee confusion about the many healthcare options, and how these plans and programs work, as well as the increased hit on family income, have resulted in low utilization of programs designed to reduce out-of-pocket costs.
What’s an employer to do?
One solution is to implement a transparency rewards program. These programs both educate employees about the fact that they should price shop for many healthcare services, and encourage them to choose lower-cost options by putting money back in their pockets.
These rewards programs are becoming increasing popular. In fact, a Society for Human Resource Management survey showed that 60% of organizations have implemented one. And yes, it may seem counterintuitive to offer monetary rewards to lower expenses. However, employers find that when employees are incentivized to use their benefits, they are more likely to make cost-conscious healthcare choices. As the adage goes, money talks and in this case, it’s talking about saving.
Driving results with transparency rewards
Just what is a transparency rewards program? While there are different versions out there, one popular program puts a transparency provider in contact with employees and family members, who have been told by their doctors to have certain elective tests or procedures done. That company researches network providers in the employee’s geographic area and provides a written report showing three quality options, each at different price points. The employee can then make an informed decision about which provider to use.
Employees that choose a lower-cost provider save on their own out-of-pocket costs and often directly save the employer money as well. After all, who wouldn’t prefer to pay 20% of $4,000 versus 20% of $15,000, all things being equal?
But imagine if employees are then further rewarded by their employer for selecting the lowest-cost provider identified through the transparency service — with cash back in their pockets or other rewards. Employees are then not only saving money, they are making money from their informed healthcare decision. Data from DirectPath has found that employers with rewards programs have higher utilization rates of their transparency services compared to customers who do not.
While not every program looks the same, employers can follow these steps to create and roll out a program that meets the specific needs of their employees.
Step 1: Get buy-in from stakeholders outside the HR department. While a rewards program can ultimately save the company thousands of dollars, there is typically a monthly fee for the service. Work with your vendor to gather data that will show the C-suite the return on a relatively low-cost investment. Keep in mind that the funding for the rewards themselves comes from the savings generated when employees select a lower-cost option for healthcare.
Step 2: Navigate HR’s bandwidth. As with most benefits programs, there are administrative and compliance complexities inherent in rewards programs. Designing, implementing and managing a comprehensive rewards program is a major undertaking and may exceed the resources of a small HR team. Outsourcing this service means a vendor can manage these details, so HR can focus on distributing the reward itself.
Step 3: Determine the incentive. As noted above, many rewards programs provide employees with a capped percentage of the savings realized from choosing a lower-cost provider. However, according to DirectPath’s
Boosting utilization
As the other old adage goes — you can lead a horse to water but you can’t make it drink. Many employers have discovered that firsthand when the programs they introduce fall flat. The key? A clear, consistent and engaging communication program that spells out for the employee, what’s in it for me?
· Make it as simple as possible. The onus should not be on the employee to figure out how the rewards program works. Educate employees on the actions they need to take, the deadlines they need to meet and any paperwork required to earn a reward.
· Use every channel. Your plan participants are individuals, and as such have their own preferences about how, when and where they want to be communicated with. To reach as many participants as possible and ensure they receive the information they need when they need it, employers should use every communication channel at their disposal—and that fits in their budget—including meetings, posters, mailings, emails and texts, webinars, etc. Don’t limit communications to the worksite; family members often account for a large portion of plan usage.
· Communicate all year round. You don’t use your benefits only once a year, so you shouldn’t communicate about them only once a year. It’s critical to remind employees of their benefits and how to use them wisely all year — while they are incurring healthcare costs but may have forgotten what services are available to support them.
A rewards program, coupled with a robust communications plan, can encourage participants to use their health plans wisely — ensuring that they get the care they need without unnecessarily straining their wallets. By helping employees save money on needed care, employers can increase job satisfaction and loyalty — driving overall productivity and performance at the company. After all, a penny saved is a penny earned, especially as the future of healthcare spending is uncertain.