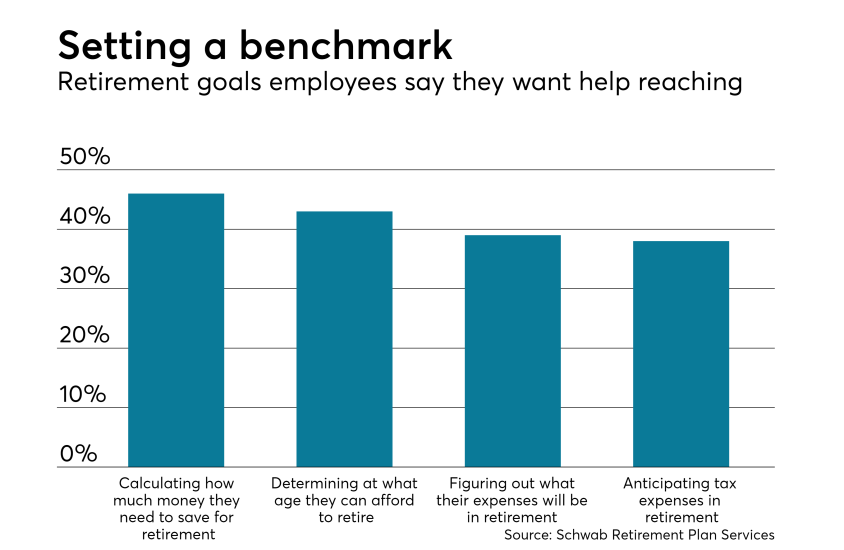
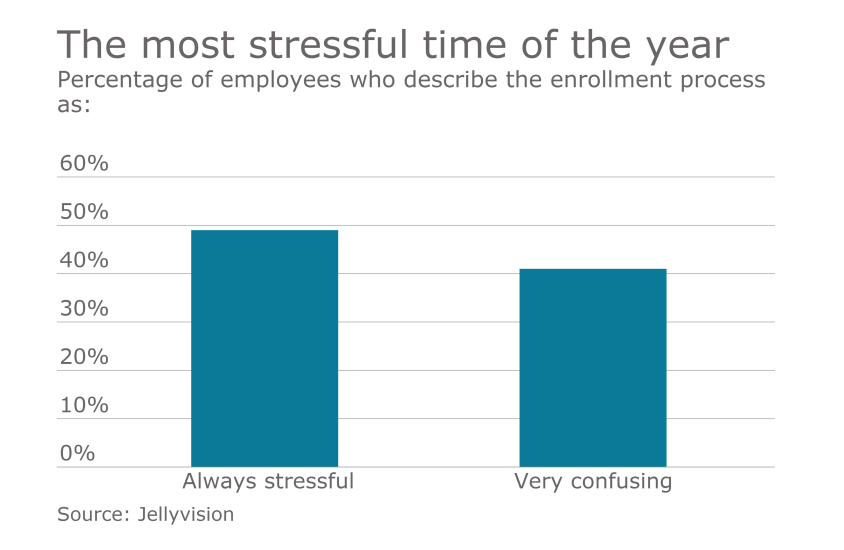
Financial wellness, recruiting tactics, direct primary care and the latest and greatest technology: Those were among the main talking points at the Workplace Benefits Renaissance, held last week in Nashville.
Brokers, employers and other benefits industry experts discussed it all while gathered during the annual conference, hosted by Employee Benefit Adviser.
Here are 10 key takeaways from the annual event.